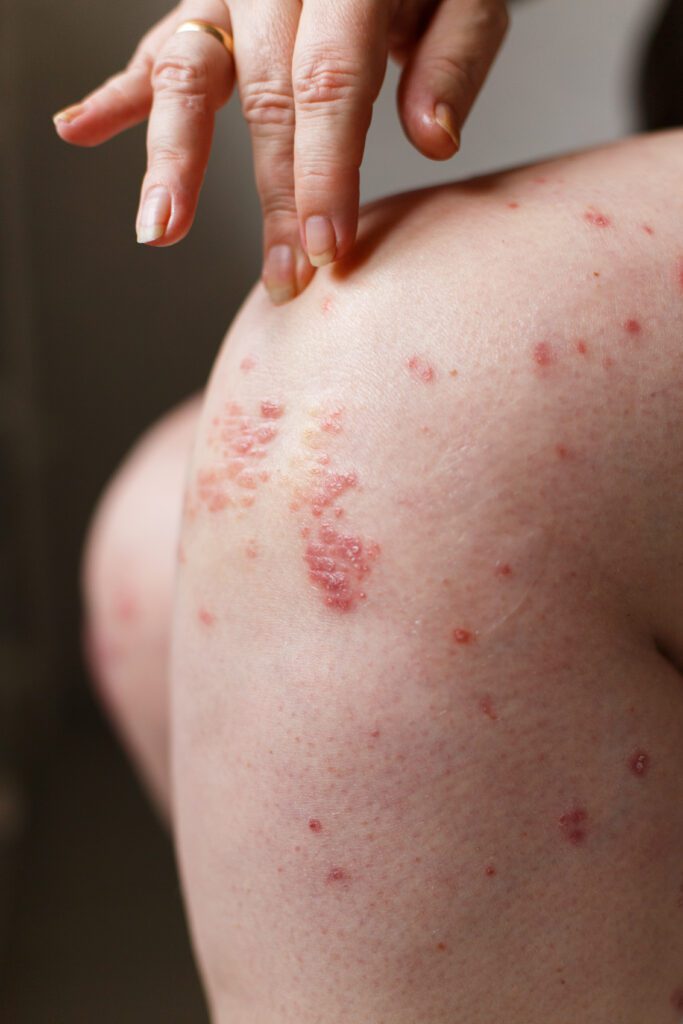
Psoriasis
Two to three percent of the world’s population suffers from psoriasis. That may not seem like a significant number, but it equals roughly 125 million people globally.
Perhaps you’re one of those people, or maybe you’re someone who loves someone with psoriasis. Either way, you want to learn more about this condition and how it is treated. Here’s a quick guide on everything you need to know about psoriasis.
What is Psoriasis?
Psoriasis is an autoimmune condition that affects the skin. Everyone’s skin cells naturally multiply to replenish the skin; however, if you have psoriasis, this process occurs up to 10 times faster than it does in the average person.
With so many excess skin cells forming, they start to build up into red patches and scaly, white skin on your body. These patches can appear all over the body but are most common on the knees, elbows, lower back, and scalp.
What are the Causes of Psoriasis?
Experts are unclear on the reasons why people develop psoriasis. However, they do know that your genetics and your immune system will factor in.
This isn’t to say that psoriasis is passed on from family member to family member, though. It’s linked to genetics, but you can develop it without having a parent or grandparent with the condition.
It could also be that your psoriasis is triggered by skin injury, stress, or particular medications. Experts have also found a link between infections –particularly strep-based ones –and the development of psoriasis.
Symptoms of Psoriasis
There’s no one-size-fits-all list of psoriasis symptoms. However, while those with the condition can experience a range of symptoms, these five are the most common:
- Red patches of inflamed skin, which are often topped by scaly patches of white or silver skin
- Skin that is painful and itchy, to the point where it cracks and/or bleeds
- Skin that bleeds after being scratched
- Patches of scaly skin on the scalp
- Discoloration of the fingernails and/or toenails; nails may also break or crumble, or they may fall off at the nail bed
About 30 percent of people with psoriasis will also suffer from psoriatic arthritis. This inflammatory condition tends to arise a decade after psoriasis and causes achy, swollen joints, stiffness, fatigue, and other symptoms.
How is Psoriasis Diagnosed?
Even if you see yourself in the description of symptoms above, it will take a doctor to diagnose you with psoriasis. They will likely run through a similar list of questions to confirm that you have, indeed, experienced psoriasis symptoms. They may also ask if you’ve experienced major stress or illness recently, or if you have a relative with psoriasis, as these factors can further confirm your diagnosis.
If you are having a flare-up at the time of your appointment, your doctor may also take a sample of the skin cells in the area. They can inspect this under a microscope, as it can confirm that you do, indeed, have this autoimmune condition.
What is the Treatment for Psoriasis?
There is no single cure for psoriasis, but there are more therapies than ever to help soothe your flare-ups. And it is vital that you seek treatment for your psoriasis –even a mild case shows that you have inflammation in your body, which can cause other diseases to develop.
You should always speak to an expert before embarking on a treatment plan. However, here are some potential routes that you may go down to help keep your psoriasis in check.
Balanced Gut Health for Psoriasis
One way that you can reduce your psoriasis symptoms—as well as the inflammation it causes in the body –is by balancing your gut health. That does not mean that you need to change up your diet completely; instead, you may consider taking a probiotic to replenish your gut’s store of these important bacteria.
Your body contains approximately 100 million microbes, and they play a vital role in your overall health. The gut-based bacteria helps strengthen your immune system, ward off germs, and digest your food. Your microbiome can even promote positive mood and mental processes, should it be balanced.
However, an unbalanced gut may be a factor in psoriasis. One study found that those with psoriasis had less diversity in their microbiome than those without the autoimmune condition.
Experts have yet to definitively say if probiotics are a bona fide treatment for psoriasis. However, results so far have been promising. And there’s no risk in trying, as probiotics have already been tested and deemed safe for our use, whether we have an autoimmune condition or not.
Hormone Balance and Psoriasis
Another potential treatment for psoriasis revolves around hormones. Some experts believe that hormones play a role in psoriasis flare-ups because psoriasis tends to be at its worst during major hormonal changes, such as puberty and menopause.
Once again, it’s important to speak to a doctor or skincare expert before starting any type of psoriasis treatment. But you may decide together that hormone therapy is the right course of action for you. As the name suggests, this treatment aims to restore hormonal balance and fixing your hormone levels will do more for you than just assuage your scaly patches of skin. It can also help with weight loss, moods, anxiety, and poor sleep. So, if you’ve been experiencing those symptoms alongside your psoriasis, it could be a major sign that your hormones need balancing.
When to See a Doctor for Psoriasis
If you’re reading this guide to psoriasis and seeing yourself in the description, then you should be seeing your doctor as soon as possible. They can make a final diagnosis and get you on the path to treatment so that your skin doesn’t bother you as much as it is right now. Feeling relief is important, and you can with the proper care.
EvexiPEL certified practitioners are highly trained in integrative medicine therapies, including optimizing gut health and hormonal balance. If you are plagued by psoriasis, find an EvexiPEL Certified Practitioner near you.